How long does it take to pump enough milk for storage?
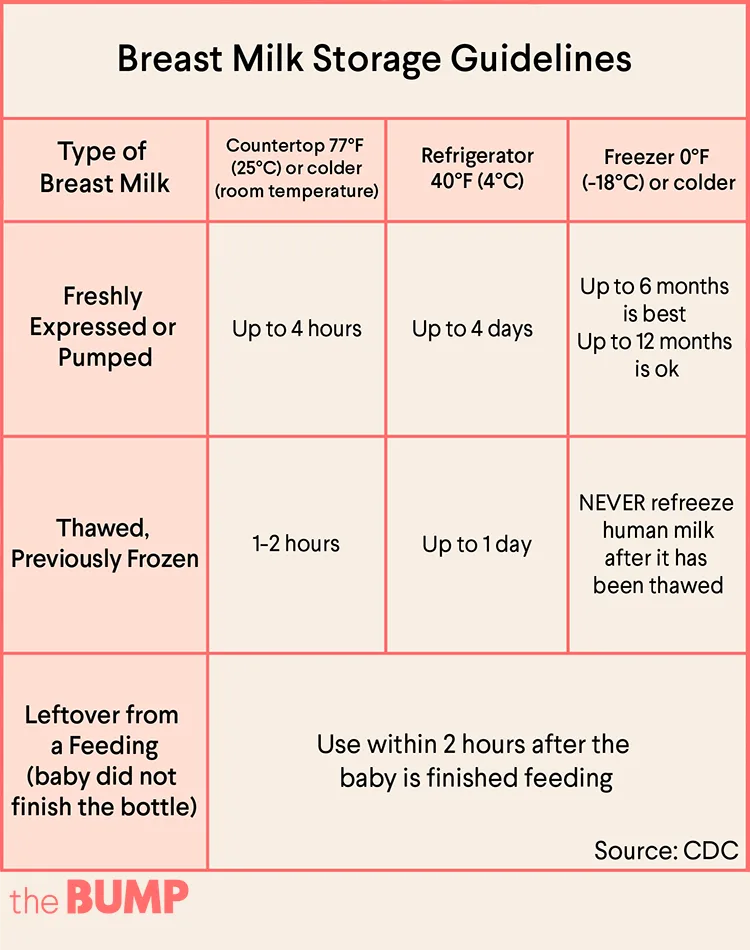
What is the 5 5 5 rule for breast milk?
She also recommends the 5:5:5 rule, which can be a quick lifesaver for moms to reference. “Something I recommend to moms is the 5-5-5 rule,” Pawlowski says. “Try and use milk within five hours at room temperature, five days if in the refrigerator, and five months if in the freezer.”
How many ounces is 15 minutes of breastfeeding?
“`html
How we measure a milk supply is fairly arbitrary, because a milk supply is always adjusting and changing based upon the stimulation it has received over the previous hours and days. Directly nursing parents do not actually “know” their milk supply and that’s normal. A healthy milk supply is not measured by the exact number of ounces, but rather by its ability to meet the growth needs of the unique baby it is responding to.
Pumps have become more accessible (every insurance company is required to cover it by 2015 under the Affordable Care Act) and effective (they are quiet, comfortable, and they work). Over the years of use, it is becoming clear that a milk supply doesn’t require a baby’s sucking input to be protected and promoted.
It feels important to contextualize milk supply here before I simply categorize supply into three overly simplified ranges. Sustaining the life of the baby you birthed with your lactating mammaries is an ancient human physiological act. Much like birth, the body knows what to do and we opt to intervene often because the body isn’t always safe doing what it is trying its best to do.
When speaking about milk supply, there is only one question that guides us toward “normal milk supply.” Is there enough milk for the baby to grow? Once, that was the only measurement of milk supply. There is so much risk and uncertainty in that, it makes sense that modern parents opt towards having more data to guide their decision making.
So, it is with that context, that I present my proposal of how to best understand a lactating parent’s unique, ever changing milk supply. Your milk supply is responsive to the stimulations it has received over the past 3-5 days. Here we use the unit of measure of ounces per twenty four hours which also helps us estimate the ounces produced per hour. A milk supply will adjust to its “average” by about 4-6 postpartum.
In the past 3 days, with ___ # stimulations, my milk supply was ____oz in the past 24 hours.
If you’re exclusively pumping and not nursing at all, and do not intend to, there is a shift in mindset and management of supply. Refer to “Special Circumstances: Exclusive Pumping”. If you’re nursing at all, here’s how to gauge your milk supply since you can’t directly measure it for 24 hours.
Bossy Boobs: When your baby doesn’t want to eat and your boobs do want the baby to eat, you have a problem: to pump or not to pump.
Reasons To Suspect Low Supply:
- First
When troubleshooting low supply, we take a four-pronged approach that follows the Breastfeeding Rules:
- 3 Ways
Any change in supply and demand takes about three to five days to make any change, with the full effect seen in two weeks. Pumping after breastfeeding is a helpful way to fully drain your breasts and send your body a message to make more milk. This is the extra demand that will hopefully yield a higher supply.
Pumping Tips:
- Choose a supply boosting pumping strategy:
Hormone manipulation comes in two ways: prescriptions and herbal supplements. There is
“`
How long after pumping do I have to store milk?
“`html
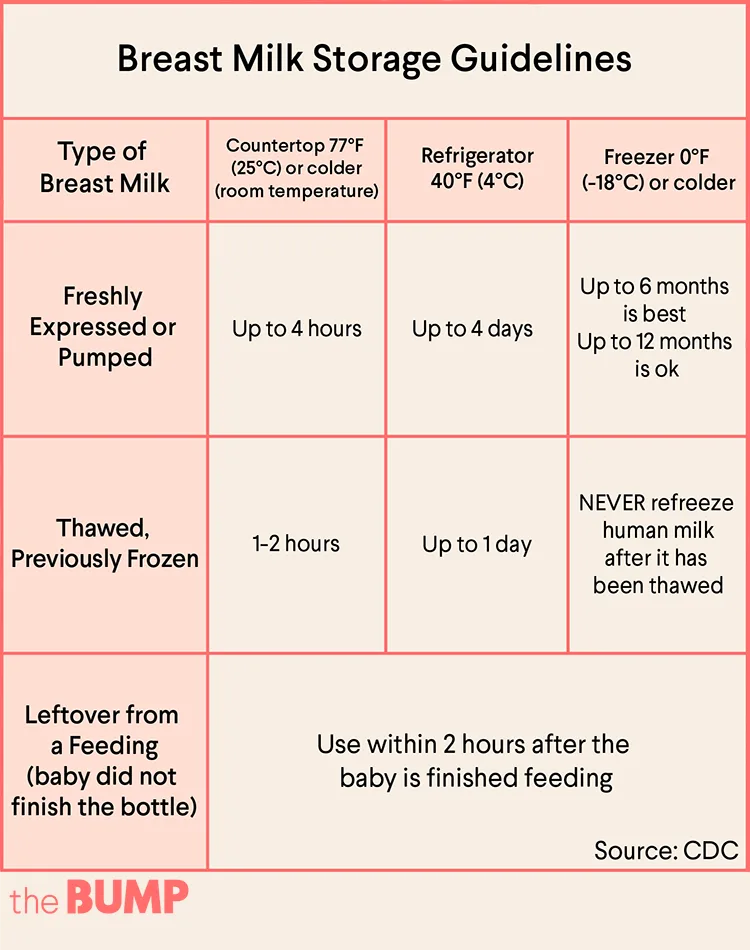
Various factors affect how long human milk can be stored safely. The storage and preparation techniques recommended can help maintain the safety and quality of expressed breast milk for the baby’s health. This page provides information for storing human milk at different temperatures and for preparing human milk after storage.
Wash your hands well with soap and water. If soap and water are not available, use an alcohol-based hand sanitizer that contains at least 60% alcohol.
Mothers can express breast milk by hand or with a manual or electric pump. If using a pump, inspect the pump kit and tubing to make sure it is clean. Discard and replace moldy tubing immediately. If using a shared pump, clean pump dials, power switch, and countertop with a disinfectant wipe.
Use breast milk storage bags or clean, food-grade containers to store expressed breast milk. Make sure the containers are made of glass or plastic and have tight fitting lids. Never store breast milk in disposable bottle liners or plastic bags that are not intended for storing breast milk.
Freshly expressed or pumped milk can be stored:
Do you have other questions, such as where to store breast milk at work or what to do when the power goes out? Visit Frequently Asked Questions.
Clearly label breast milk with the date it was expressed. Do not store breast milk in the door of the refrigerator or freezer. Storing it further inside will help protect the breast milk from temperature changes when the door opens and closes.
If you don’t think you will use freshly expressed breast milk within 4 days, freeze it right away. This will help to protect the quality of the breast milk.
When freezing breast milk:
If you deliver breast milk to a childcare provider, clearly label the container with the child’s name. Talk to your childcare provider about any other requirements for labeling and storing breast milk.
Breast milk can be stored in an insulated cooler with frozen ice packs for up to 24 hours when traveling. At your destination, use the milk right away, store it in the refrigerator, or freeze it.
Remember: First in, first out. Always thaw the oldest breast milk first. Over time, the quality of breast milk can decrease.
You can thaw your breast milk by putting the container in the refrigerator overnight, in warm or lukewarm water, or under lukewarm running water. Never thaw or heat breast milk in a microwave. Microwaving can destroy nutrients in breast milk and create hot spots, which can burn a baby’s mouth.
If you thaw breast milk in the refrigerator, use it within 24 hours. Start counting the 24 hours when the breast milk is completely thawed, not from the time when you took it out of the freezer. Once breast milk is brought to room temperature or warmed, use it within 2 hours.
Never refreeze breast milk after it has thawed. Breast milk does not need to be warmed. It can be served room temperature or cold.
If you decide to warm the breast milk, here are some tips: Swirl the breast milk to mix the fat, which may h
“`
When should I pump to build a stash?
“`html
r/breastfeeding
This is a community to encourage, support, and educate parents nursing babies/children through their breastfeeding journey. Partners seeking advice and support are also welcome here.
Members
Online
Not sure if my title makes sense .. but basically I understand you’re not supposed to pump unless the baby is eating (bottle from dad, etc.) Otherwise you risk creating an oversupply.
But if you want to share the burden of feeding with a partner by building a stash, and you want to breastfeed exclusively, how do you go about doing that??
It seems like the options are either create an oversupply OR have dad use formula while you pump? Am I missing something?
Archived post. New comments cannot be posted and votes cannot be cast.
“`
How quickly does milk replenish after pumping?
“`html
After pumping, moms often ask how long after pumping breasts refill. True milk production would take much more. In this guide, refilling will be discussed with recommendations to help in maximizing milk flow supporting a more comfortable and smoother feeding routine.
Breast milk is constantly replenished. Your body will automatically begin producing more milk almost immediately after you finish nursing or pumping. The constant production process does increase your milk levels, but in most cases, the growth may be minimal over the longer term. Milk can be produced faster if the breasts have less of it to provide, but when it builds up in the breast, the rate of production drops. This is technically where it is replenishing its reserves, so you could argue they are never “dry”.
Most mothers can see that milk production is building back up within 20–30 minutes of a pumping session. A fuller refill will take longer, usually about an hour or two, depending on how hydrated you are, your diet, and how frequently you pump or nurse. Since your body is always making milk, you rarely need to wait a specific amount of time to pump or feed again.
Knowing how long after pumping do breasts refill will better prepare you to make sure your baby gets enough for your baby’s next feed. Here’s how quickly breasts refill:
Yes, and here are several ways you can encourage quicker milk replenishment after pumping:
- Stay Hydrated
Ensure that you take in enough water throughout the day. You can shoot for at least 8–10 glasses of water a day and other fluids if you feel thirsty or need to pump more often. Dehydration will slow down milk production, so drinking water regularly is very important. - Eat a Healthy, Balanced Diet
Your body needs the essential nutrients required to produce milk, so a healthy, well-balanced diet is crucial. Add high-protein foods, such as lean meats, eggs, and legumes, as well as healthy fats from avocados, nuts, and olive oil. Carbohydrates, especially whole grains, give you the energy to maintain your milk supply. Some foods may have a lactogenic effect to enhance milk production. Many lactating mothers like oats, brewer’s yeast, and herbs like fenugreek and blessed thistle. - Pump or Nurse Frequently
Frequent and consistent milk expression will tell your body to produce more milk. Pump at regular time intervals to maintain the cycle of milk production. Exclusive pumping moms will often pump every 2–3 hours, much like a newborn’s feeding schedule, which keeps levels high. The Momcozy M9 Hands-Free Breast Pump will help you maintain and improve a good milk supply as it gives you the ability to pump to your schedule, which is fundamental in the preservation of milk supply over time.
High Efficiency
Multiple Modes
APP Control
Long Battery
Massage Your Breasts and Compress
A gentle massage or compression of the breasts while pumping stimulates flow and can increase production more rapidly. Massaging both before and during pumping assists the.
“`
How long after pumping do I have to store milk?
“`html
Various factors affect how long human milk can be stored safely. The storage and preparation techniques recommended can help maintain the safety and quality of expressed breast milk for the baby’s health. This page provides information for storing human milk at different temperatures and for preparing human milk after storage.
Wash your hands well with soap and water. If soap and water are not available, use an alcohol-based hand sanitizer that contains at least 60% alcohol.
Mothers can express breast milk by hand or with a manual or electric pump. If using a pump, inspect the pump kit and tubing to make sure it is clean. Discard and replace moldy tubing immediately. If using a shared pump, clean pump dials, power switch, and countertop with a disinfectant wipe.
Use breast milk storage bags or clean, food-grade containers to store expressed breast milk. Make sure the containers are made of glass or plastic and have tight fitting lids. Never store breast milk in disposable bottle liners or plastic bags that are not intended for storing breast milk.
Freshly expressed or pumped milk can be stored:
Do you have other questions, such as where to store breast milk at work or what to do when the power goes out? Visit Frequently Asked Questions.
Clearly label breast milk with the date it was expressed. Do not store breast milk in the door of the refrigerator or freezer. Storing it further inside will help protect the breast milk from temperature changes when the door opens and closes.
If you don’t think you will use freshly expressed breast milk within 4 days, freeze it right away. This will help to protect the quality of the breast milk.
When freezing breast milk:
If you deliver breast milk to a childcare provider, clearly label the container with the child’s name. Talk to your childcare provider about any other requirements for labeling and storing breast milk. Breast milk can be stored in an insulated cooler with frozen ice packs for up to 24 hours when traveling. At your destination, use the milk right away, store it in the refrigerator, or freeze it.
Remember: First in, first out. Always thaw the oldest breast milk first. Over time, the quality of breast milk can decrease.
You can thaw your breast milk by putting the container in the refrigerator overnight, in warm or lukewarm water, or under lukewarm running water. Never thaw or heat breast milk in a microwave. Microwaving can destroy nutrients in breast milk and create hot spots, which can burn a baby’s mouth.
If you thaw breast milk in the refrigerator, use it within 24 hours. Start counting the 24 hours when the breast milk is completely thawed, not from the time when you took it out of the freezer. Once breast milk is brought to room temperature or warmed, use it within 2 hours.
Never refreeze breast milk after it has thawed. Breast milk does not need to be warmed. It can be served room temperature or cold.
If you decide to warm the breast milk, here are some tips: Swirl the breast milk to mix the fat, which may h
“`
What is the 5 5 5 rule for breast milk?
She also recommends the 5:5:5 rule, which can be a quick lifesaver for moms to reference. “Something I recommend to moms is the 5-5-5 rule,” Pawlowski says. “Try and use milk within five hours at room temperature, five days if in the refrigerator, and five months if in the freezer.”
When should I pump to build a stash?
“`html
r/breastfeeding
This is a community to encourage, support, and educate parents nursing babies/children through their breastfeeding journey. Partners seeking advice and support are also welcome here.
Members
Online
Not sure if my title makes sense .. but basically I understand you’re not supposed to pump unless the baby is eating (bottle from dad, etc.) Otherwise you risk creating an oversupply.
But if you want to share the burden of feeding with a partner by building a stash, and you want to breastfeed exclusively, how do you go about doing that??
It seems like the options are either create an oversupply OR have dad use formula while you pump? Am I missing something?
Archived post. New comments cannot be posted and votes cannot be cast.
“`